Dr. Gillaspy has taught health science at University of Phoenix and Ashford University and has a degree from Palmer College of Chiropractic.
Parathyroid Gland: Calcium Metabolism, Osteoclasts & PTH
Table of Contents
- Parathyroid Glands
- Parathyroid Hormone (PTH)
- Osteoclasts and Osteoblasts
- Calcium Balance
- Lesson Summary
- Learning Outcomes
The thyroid gland is an endocrine gland that sits at the base of your neck. When we flip the thyroid gland over and take a look at its back side, we see that the posterior surface of the thyroid gland contains tiny masses of glandular tissue that serve an entirely different function from that of the thyroid. In this lesson, we will learn about these small endocrine glands, referred to as the parathyroid glands, and the role they play in balancing calcium levels within the body.
 |
When we look at the thyroid gland, we see that it roughly resembles a butterfly with its two lobes that wrap around the trachea, or windpipe; so, if we think of the thyroid gland as a butterfly, we can think of the parathyroid glands as tiny spots on the butterfly's wings.
We typically have four parathyroid glands that sit on the posterior surface of the thyroid gland. These glands are quite small - about the size of a grain of rice - and appear somewhat unimpressive. In fact, in the early days of medicine, their importance was not understood, and if a patient needed to have a surgery on his or her thyroid gland, the surgeon was apt to remove the parathyroid glands along with the thyroid tissue. This would often result in the patient's death because the surgeons did not realize that the hormones produced by the parathyroid glands play a necessary role in regulating calcium levels in the body.
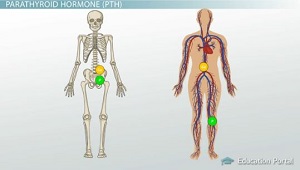
A hormone that comes from the parathyroid glands is conveniently called a parathyroid hormone (PTH). So, we see that parathyroid hormone is defined as a hormone produced by the parathyroid glands that regulates the amount of calcium and phosphorus in the body.
Calcium is an important ion that has a wide variety of effects on the body. We usually think of calcium when we think of bone formation, but it's also important for proper muscle contraction and proper cell membrane permeability.
Phosphorus, like calcium, is needed for bone formation. Among other things, it combines with lipids to form a major structural component of all cell membranes, which we know as phospholipids.
Obviously, when we talk about bone formation, we're talking about our bony skeleton. It's easy to think of your skeleton as the part of your body that provides support and gives you your basic height and shape. What we don't always think about as quickly when we talk about the bony structures is that they hold a large reserve of calcium and phosphate.
These two minerals can be found floating around in your bloodstream. The amount that is in your blood at any given time needs to be closely regulated and maintained within a very narrow limit in order for your body to be in homeostasis, or internal balance.
If the body needs more of these minerals, it turns to the reserves found in the bony skeleton, and if there are too many of the minerals present in the blood, the minerals are deposited in the bone. Therefore, we see that bone is constantly being broken down and built up to keep the blood levels within a normal range. This is done through the action of osteoclasts and osteoblasts.
 |
Osteoclasts are cells that break down bone. Osteoblasts do the opposite action, and therefore, we see that osteoblasts are cells that make bone. You can keep these straight by thinking of osteoclasts as chewing bone as it breaks it down and osteoblasts as building bones.
So, when we put everything together, we see that a decrease in blood calcium levels triggers the release of parathyroid hormone, which stimulates osteoclasts to break down bone. This frees calcium to enter the blood, restoring the level to normal.
One thing that's very apparent when learning about the endocrine system is that the release of a hormone is often dependent on maintaining homeostasis - and this is the case with parathyroid hormone. We see that the secretion of parathyroid hormone happens when blood calcium levels drop too low. So, you might be wondering: what happens if blood calcium levels get too high?
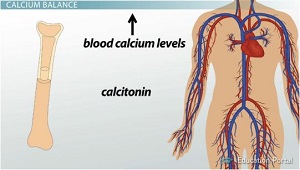
This gives us an opportunity to reintroduce a hormone we previously learned about called calcitonin. Calcitonin is a hormone secreted by the thyroid gland that lowers blood calcium levels.
In other words, parathyroid hormone puts calcium in the blood, and calcitonin clears it out of the blood. It's almost as if these two hormones, parathyroid hormone and calcitonin, are constantly locked in a tug-of-war match.
So, we see that when blood calcium levels are too high, parathyroid hormone is inhibited, and calcitonin is released. The calcitonin stimulates osteoblasts to build up bone. This removes excess calcium from the blood and brings the blood calcium level back to a normal level.
 |
To this point, we have only talked about parathyroid hormone in regards to bone breakdown. However, it's good to note that parathyroid hormone affects more than just the bones. It can also raise blood calcium levels by stimulating calcium reabsorption in the kidneys. When calcium is reabsorbed in the kidneys, it stays in the body and is not excreted in the urine. Therefore, parathyroid hormone not only raises blood calcium levels by breaking down bone, it also stimulates the kidneys to reabsorb calcium.
Let's review. Parathyroid hormone (PTH) is a hormone produced by the parathyroid glands that regulates the amount of calcium and phosphorus in the body.
Secretion of parathyroid hormone is stimulated by low blood calcium levels and inhibited by high blood calcium levels. Therefore, when blood calcium levels are too low, parathyroid hormone is released, which stimulates the breakdown of bone. This frees calcium to enter the blood, restoring the level to normal.
Osteoclasts are the cells that break down bone. Parathyroid hormone can also act on the kidneys to raise blood calcium levels. It does this by stimulating calcium reabsorption by the kidneys, so more calcium stays in the body and less is excreted through the urine.
The antagonist to parathyroid hormone is calcitonin. If blood calcium levels get too high, parathyroid hormone is inhibited and calcitonin is released. This stimulates osteoblasts, which are cells that make bone.
Following this lesson, you should have the ability to:
- Describe the structure and function of the parathyroid glands
- Explain how parathyroid hormone, calcitonin, osteoblasts, and osteoclasts function together to regulate the body's calcium levels
- Summarize the antagonistic actions of parathyroid hormone and calcitonin
- Understand the two ways parathyroid hormone can increase blood calcium levels
Register to view this lesson
Unlock Your Education
Become a Study.com member and start learning now.
Become a MemberAlready a member? Log In
BackResources created by teachers for teachers
I would definitely recommend Study.com to my colleagues. It’s like a teacher waved a magic wand and did the work for me. I feel like it’s a lifeline.






